Phone: 326 332 991
orthopeadics - procedures and examinations
MUDr. Daniel Horáček
ORTHOPAEDICS: TOTAL KNEE REPLACEMENT
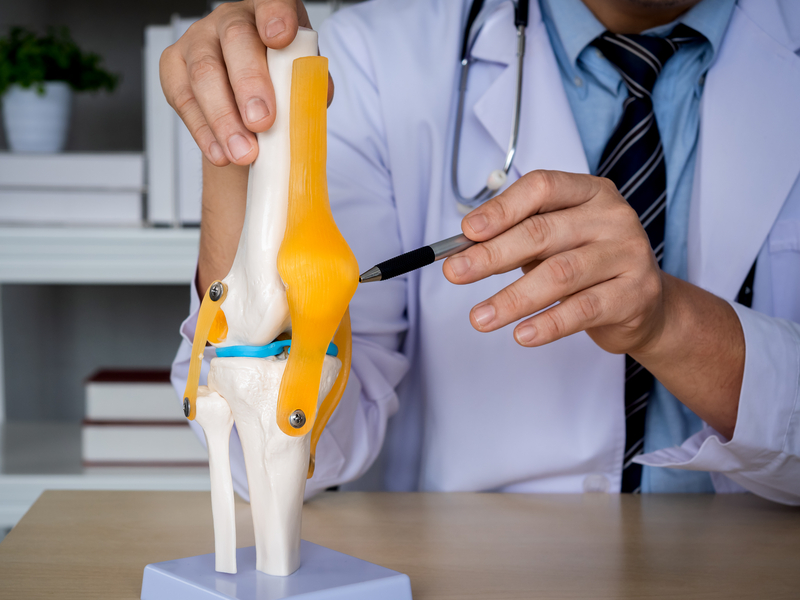
Anatomy of the knee joint
The knee joint is made up of the femur, tibia, fibula and patella. The sliding surfaces of the joint are covered by hyaline cartilage. The stability of the knee joint is due to the articular ligaments, menisci, muscles and joint capsule. The nerves and blood vessels supplying the lower limb run in the immediate vicinity of the joint.
Disorders and arthrosis of the knee (gonarthrosis)
Various developmental, post-traumatic and post-inflammatory conditions can lead to damage to different parts of the joint. These conditions lead to arthrosis of the knee.
The symptoms of this disease are first pain on exertion, restriction of movement, stiffness of the joint and then rest pain. Gradually, the limb deforms, in particular the axis of the limb changes.
Treatment of gonarthrosis
The treatment itself can be divided into conservative procedures, i.e. non-operative and operative procedures.
In the early stages of gonarthrosis, we use mainly pharmacological and rehabilitation procedures, with a strong emphasis on appropriate choice of sports activities.
Cycling and swimming are particularly suitable. An equally important part of the treatment is the control of the patient's weight.
Surgical treatment includes arthroscopic treatment and open surgical techniques.
Arthroscopic treatment can be used for meniscal damage, treatment of chondral defects and other knee damage.
Open surgical techniques mainly include osteotomies to correct the limb axis and implantation of total knee arthroplasties. When deciding on the indication for a particular surgical solution, the patient's difficulties indicating the degree of joint damage are always decisive.
Artificial joint - alloplasty - total knee arthroplasty (TEP)
Knee alloplasty is the replacement of a damaged joint with an implant. The femoral and tibial components of a total knee arthroplasty are most often made of a metal alloy and fixed with bone cement. A polyethylene insert is the key part of the total hip replacement.
Preoperative preparation
Prior to total joint replacement, the patient undergoes a series of examinations, coordinated by his or her treating physician throughout the preoperative preparation.
An integral part of the preoperative preparation is also the examination of inflammatory foci to exclude endogenous sources of infection in order to reduce the risk of postoperative complications. Preoperative consultation with the anesthesiologist of our Clinic is also an advantage.
Basic scheme of preoperative examination:
1/ exclusion of inflammatory foci (foci)
- swabbing of the nose and throat for culture
- examination of urine (in women better catheterized urine)
- dental examination
- gynaecological examination
2/ preoperative internal examination including laboratory tests
Usually performed by the attending general practitioner in collaboration with an internist three weeks before surgery,
The aim is to ensure the functional stability and reserves of the patient to cope with the surgery and postoperative rehabilitation. Ensure proper safe adjustment of permanent medication if needed.
Before surgery, special attention is paid to adjust the dosage of blood thinners, diabetes medications. Cannot perform surgery and take blood thinners at the same time.
Standard required examination:
- ECG, RtgS+P,
- Blood tests KO, INR APTT, Urea, creatinine, Na, K, Cl, bili, ALT AST, glucose, CRP
- Urinalysis M+S
- Other investigations are required in case of other chronic diseases.
Admission to surgery: the day before surgery at 11.00 a.m. / Patient can have breakfast and drink fluids on the day of admission / Patient should take his/her medication with him/her on the day of admission, if any
Surgery
Before surgery - the surgeon will give the patient a detailed briefing on the surgical procedure, alternatives to surgery and post-operative treatment.
The time the patient spends in the operating room is individual. Upon arrival at our facility, an anesthesiologist will visit the patient and discuss with the patient the appropriate method of anesthesia and postoperative analgesia During surgery and immediately after surgery, we use procedures and systems that conserve blood loss.
Postoperative recovery
After surgery, the patient is followed in the post-operative ward, where their condition is continuously monitored.
Further treatment then takes place in the monitored beds of our facility, where the patient is cared for by a team of experienced nurses, orthopaedic surgeons and physiotherapists. The patient has his/her own personal physiotherapist throughout the stay.
The average hospital stay after surgery is one week. During this time, under the guidance of the physiotherapists, the patient learns basic self-sufficiency and how to walk on flat ground and up stairs.
After this time, the patient is usually able to be discharged for home treatment. Depending on the course of treatment and the provision of home care after discharge, the patient may remain in our Clinic for the follow-up treatment or we may arrange for transfer to an appropriate rehabilitation institute or spa.
For a detailed description of post-operative rehabilitation care during hospitalization see. "Rehabilitation standards in orthopaedics".
Complications and risks
You will be informed in detail about all risks by your doctor during the outpatient examination. The doctor will also be happy to answer any further questions you may have.
Regimen recommendations for patients after total replacement can be found clearly on our website and will be repeatedly reminded during your stay with us.
See. Informed Consents

Anatomy. The knee joint consists of the femur, tibia, fibula and patella.
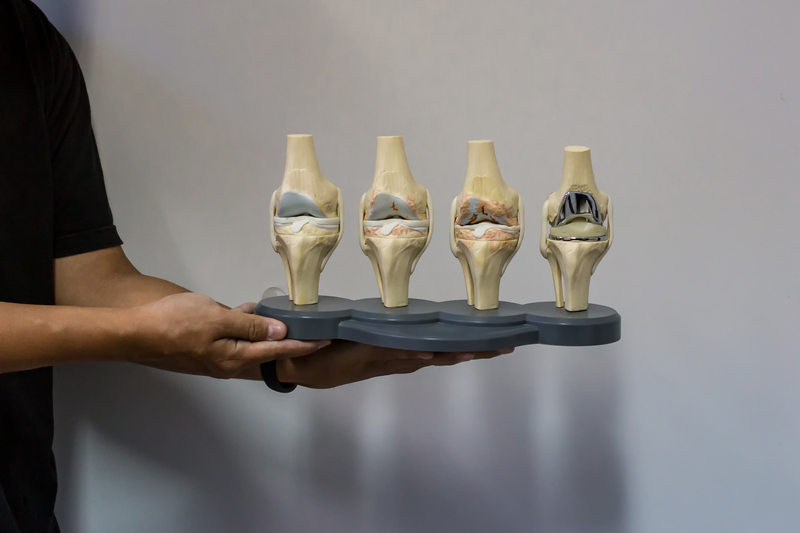
Arthritis of the knee. An anatomical model of the knee showing the progression of knee osteoarthritis that ends in total knee replacement surgery.

Disease. Manifestations are first pain on exertion, limitation of movement, stiffness of the joint and then resting pain.